Chemo May Spread Breast Cancer and Trigger More Aggressive Tumors
July 11, 2017 | Author: Susan Silberstein, PhD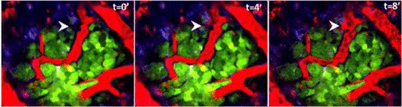
I have written about the dangers of chemotherapy before. A study published last year in Breast Cancer Research confirmed that, in addition to suppressing immunity during cancer treatment, chemotherapy can actually cause long-term damage to the immune system.
In 2012, researchers at the Fred Hutchinson Cancer Research Center in Seattle published a prostate cancer study explaining that chemotherapy can boost cancer growth. The expression of a certain protein in the prostate tumor microenvironment was shown to lessen the cell-kill effects of chemotherapy, thereby promoting cancer cell survival and disease progression.
Last fall, British researchers looked at the number of cancer patients who died within 30 days of starting chemotherapy and found results suggesting that, for many, the treatment was the cause of death, rather than the cancer.
And just last week, a study published in the journal Science Translational Medicine, offered additional insight into how chemotherapy can cause cancer to spread and trigger more aggressive new tumors. Dr. George Karagiannis and colleagues at the Albert Einstein College of Medicine in New York released their research on the impact of chemo drugs on breast cancer patients showing that the drugs increased the chance of cancer spreading to other parts of the body. The researchers found that, while shrinking tumors, chemotherapy also increases the number of ‘doorways’ opening in blood vessels (a process called “intravasation”) by which cancer can metastasize.
Patients often express concern that surgery could increase risk for spread of cancer. The new study presents evidence that chemotherapy can too. Groups of cells collectively known as “tumor microenvironment of metastasis” (TMEM, a known predictor of metastasis in breast cancer patients) can serve as gateways for tumor cells entering the blood stream. The Einstein scientists discovered that several types of chemotherapy can increase the amounts of TMEM complexes and circulating tumor cells in the bloodstream. In fact, the study authors found that the number of doorways was increased in 20 patients receiving two common chemotherapy drugs (paclitaxel after doxorubicin plus cyclophosphamide). They also discovered that in mice with breast cancer, chemotherapy increased the number of cancer cells circulating in the body and in the lungs.
The researchers suggested that women receiving chemotherapy to shrink tumors prior to breast surgery be monitored during therapy to check if cancer cells are starting to circulate and if doorways are emerging. If this is found to be the case, they recommended discontinuing chemo before surgery. The scientists are currently planning more extensive trials to address the issue and also to investigate chemotherapy-induced metastatic spread in other cancers.
As Chris Wark has said, chemotherapy is often only a short-term solution to a long-term problem.And whether triggered by chemo or not, I believe that testing for circulating tumor cells is one of the best tools we have for predicting the risk of cancer spread and for monitoring whether the therapeutic program a patient is following is doing an efficient enough job to control that.
Join the conversation: Ask Holistic Cancer Coach Facebook Group
References:
[1] De Graaf M. Chemotherapy could cause cancer to SPREAD and grow back even more aggressive, new study claims. The Daily Mail, 5 July 2017 http://www.dailymail.co.uk/health/article-4669152/Chemotherapy-cause-cancer-SPREAD-new-study-says.html
[2] http://www.chrisbeatcancer.com/chemo-may-spread-breast-cancer-and-trigger-more-aggressive-tumors/
[3] http://www.chrisbeatcancer.com/chemotherapy-backfire-boost-cancer-growth-study/
[5] http://stm.sciencemag.org/content/9/397/eaan0026
[7] Karagiannis GS, Pastoriza JM,Wang Y, Harney AS, et al. Neoadjuvant chemotherapy induces breast cancer metastasis through a TMEM-mediated mechanism. Science Translational Medicine 05 Jul 2017: Vol. 9, Issue 397
[8] Knapton S. Chemotherapy may spread cancer and trigger more aggressive tumours, warn scientists. The Telegraph, 5 July, 2017.
[9] Sun Y, Campisi J, Higano C, Beer TM, et al. Treatment-induced damage to the tumor microenvironment promotes prostate cancer therapy resistance through WNT16B. Nat Med. 2012 September ; 18(9): 1359–1368. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC3677971/pdf/nihms468571.pdf
